Medical disclaimer: This article is for education only and does not provide medical advice, diagnosis, or treatment. Breast Implant Illness (BII) symptoms overlap with many conditions. If you have urgent symptoms such as chest pain, shortness of breath, high fever, or sudden neurologic changes, seek emergency care.
Breast Implant Illness Symptoms, What Research Shows about BII, and How Explant Surgery May Help
Breast Implant Illness, often shortened to BII, is a term that describes a wide range of systemic symptoms some individuals believe are connected to breast implants. Some people feel well for years after augmentation or reconstruction and then develop symptoms that do not have a clear explanation. Others notice changes sooner. Because symptoms can affect the entire body, many patients spend significant time seeking answers.
At DeRosa Plastic Surgery, Dr. Amy P. DeRosa provides consultations for patients concerned about symptoms they associate with implants and for patients considering breast implant removal (explantation). The goal is a clear, respectful evaluation that considers the whole patient, explores other possible medical causes, and discusses options based on your history and goals.
Quick navigation
- What is Breast Implant Illness?
- Common BII symptoms
- Research including Dr. Amy DeRosa’s cohort study
- Explant options and capsulectomy questions
- FAQ
- Contact DeRosa Plastic Surgery
Sitelinks: Home | Breast Implant Removal | FAQ | Reviews | Contact
What is Breast Implant Illness?
Breast Implant Illness is not one single lab test or one universally accepted diagnostic label. Instead, it is a term many patients use to describe a cluster of systemic symptoms that they feel began or worsened after receiving breast implants. These symptoms may appear soon after surgery or years later.
Professional organizations acknowledge that patients report these symptom clusters and that research is ongoing. For a general overview of breast implant safety topics, including patient reported symptoms, you can review the American Society of Plastic Surgeons (ASPS) patient safety resources:
A practical, patient first approach is to treat symptoms seriously while also recognizing that many medical issues can mimic BII. A high quality evaluation explores other causes such as thyroid disease, autoimmune disease, perimenopause, medication effects, sleep disorders, chronic infections, and more.
Commonly reported BII symptoms
BII symptoms can vary widely. Many patients describe multiple symptoms at once. Common reports include:
- Persistent fatigue
- Brain fog, memory changes, difficulty concentrating
- Joint pain and muscle aches
- Headaches or migraines
- Sleep disruption
- Anxiety, mood changes, depression like symptoms
- Hair thinning or increased shedding
- Skin rashes, itching, or sensitivity
- Digestive issues such as bloating or new food sensitivities
- Dry eyes or dry mouth
- Heart palpitations or a sense of being overstimulated
Not everyone has the same set of symptoms. If you are preparing for a consultation, it helps to write down:
- When symptoms started
- How often they occur
- How severe they feel
- Anything that triggers or relieves them
- Major health events around symptom onset (pregnancy, infection, new medications, high stress, hormonal changes)
Why might implants contribute to systemic symptoms?
Research is continuing and no single explanation fits every patient. Possible mechanisms discussed in medical literature include:
1) Inflammation and immune activation
Any implanted device can trigger immune activity. The body forms a capsule of scar tissue around the implant. For some patients, chronic inflammation related to the capsule may play a role in systemic symptoms. For others, the capsule remains soft and quiet for decades.
2) Biofilm
Biofilm is a community of bacteria that can adhere to surfaces and persist. In breast surgery, biofilm has been discussed in relation to capsular contracture. Researchers continue exploring whether biofilm may also be relevant to systemic symptom patterns in some patients.
3) Silicone exposure and particulate migration
In silicone gel implants, small amounts of silicone compounds may migrate over time. The clinical significance can vary and remains an area of study.
4) Individual susceptibility
Different people can respond differently to the same implant. Genetics, allergies, autoimmune history, hormone changes, and environmental exposures may influence risk.
The key takeaway is that BII is complex. A credible plan avoids dismissing symptoms and also avoids promising that one intervention will solve everything for everyone.
Research including Dr. Amy DeRosa
Dr. Amy P. DeRosa is a co author of a peer reviewed study titled “Breast Implant Illness: A Cohort Study”, published in Cureus in 2023. This retrospective cohort study evaluated symptom changes after breast implant explantation with total capsulectomy.
In the published cohort, the authors report that patients experienced meaningful reduction in symptom frequency and severity after surgery. The paper includes a structured symptom scoring approach and reports improvement after explantation with total capsulectomy in their cohort.
External links to the research:
- PubMed: Breast Implant Illness: A Cohort Study
- Corewell Health Scholarly Works: Listing for the cohort study
What this research helps with:
- It supports that a subset of patients report symptom improvement following explantation with capsulectomy.
- It emphasizes the value of tracking symptoms systematically rather than relying only on anecdotes.
- It adds to the growing body of literature that is shaping patient counseling and future study design.
FDA and trusted patient resources (external links)
For up to date, authoritative information on breast implant risks, labeling, and safety communications, review:
- FDA: Breast Implants
- ASPS: Breast Implant Patient Decision Checklist (PDF example)
- ASPS: BIA-ALCL FAQ
Breast implant removal (explantation) and common questions
Patients seek explantation for many reasons, including implant rupture, capsular contracture, cosmetic preference changes, lifestyle changes, and systemic symptoms they associate with implants. A consultation should clarify what is medically appropriate for you and what options align with your goals.
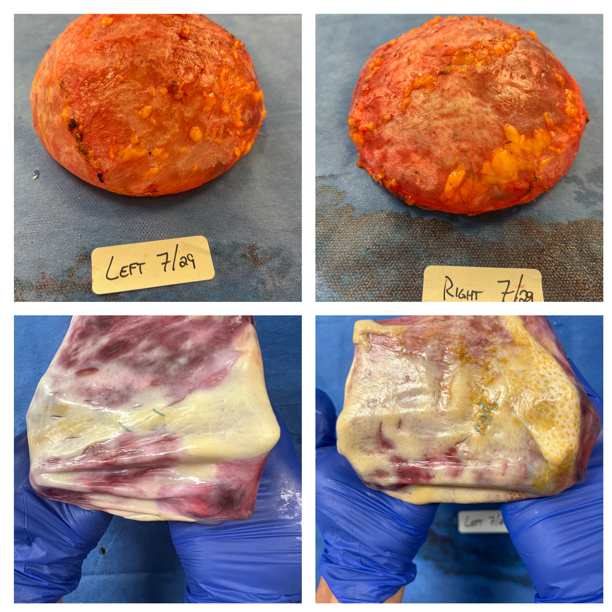
Related pages on DeRosaPlasticSurgery.com:
What recovery may look like
Recovery depends on the specific procedure performed. Patients should expect a period of limited lifting and activity, post operative follow up, and gradual improvement in swelling over weeks to months.
Your surgeon should provide a clear plan for post operative care, symptom tracking, and follow up appointments. If you are traveling for surgery, ask about travel timing, drain management if used, and how follow up is handled.
Frequently asked questions
How soon can symptoms begin?
Symptoms may appear soon after implantation or years later. There is no universal timeline. A symptom timeline is useful for evaluation.
Is BII only associated with silicone implants?
Patients report symptoms with both silicone and saline implants. The evaluation focuses on your overall health picture, implant history, and local implant findings rather than fill type alone.
What if symptoms do not improve after explantation?
Some patients report partial improvement, and some do not improve. Because symptoms overlap with other conditions, a thorough medical workup and realistic counseling are important.
How do I know if I should be evaluated for BIA-ALCL?
Late swelling, a new fluid collection, a breast mass, or significant breast changes long after implantation should be evaluated by a medical professional. Review the ASPS BIA-ALCL FAQ linked above for overview information and speak with your clinician promptly if you have concerning changes.
Next step checklist
- Gather implant records and implant cards if available.
- Document your symptom timeline and severity.
- See your primary care clinician for evaluation of other medical causes as appropriate.
- Schedule a consultation with a Dr. DeRosa.
- Discuss implant status, capsules, surgical risks, and realistic outcomes for you.
Contact DeRosa Plastic Surgery
If you would like to discuss breast implant removal or concerns about systemic symptoms, contact DeRosa Plastic Surgery:
- Phone: (248) 688-7597
- Fax: (248) 498-6060
- Address: 33200 W. 14 Mile Road, Suite 180, West Bloomfield, MI 48322
- Hours: Monday to Friday, 8:30 AM to 4:30 PM
- Contact page: https://derosaplasticsurgery.com/contact/
Related blog and education links:
Final note: If you believe your implants may be affecting your health, you deserve a thorough evaluation, clear information, and a plan that prioritizes safety and your goals.
